Discover telehealth technology for nurses explained simply. A Ghana nurse-engineer breaks down remote patient monitoring, EHR, and video care tools for bedside nurses.

| KEY TAKEAWAYS |
|---|
| ✓ Telehealth is not just video calls — it includes remote monitoring, AI triage, mobile health apps, and electronic health records. |
| ✓ Nurses are the backbone of telehealth delivery, not the afterthought. |
| ✓ Understanding basic technical concepts (bandwidth, interoperability, encryption) helps nurses troubleshoot common problems. |
| ✓ Patient safety in telehealth hinges on data accuracy, digital literacy, and informed consent. |
| ✓ Resource-limited settings like Ghana can deploy telehealth effectively with the right infrastructure and training. |
| ✓ Legal and ethical responsibilities for nurses do not change in virtual care — they expand. |
| ✓ The future belongs to nurses who combine clinical expertise with digital fluency. |
Table of Contents
Introduction: When the Ward Fits in Your Pocket
It was a Tuesday evening in the Intensive Care Unit at a district hospital in the Greater Accra Region. Three ventilated patients. Two nurses. One attending physician reachable only by phone. That night, a portable pulse oximeter connected to a central monitoring system flagged a silent desaturation in a post-operative patient before any visible symptom appeared. The nurse on duty responded within 90 seconds. That patient lived. That device — that small, connected piece of technology — was telehealth at work.
I am Abdul-Muumin Wedraogo, a Registered General Nurse with over 10 years of clinical experience across the Emergency Room, Pediatrics, ICU, and General Ward settings within the Ghana Health Service. I hold a BSc in Nursing from Valley View University, a Diploma in Network Engineering from OpenLabs, and an Advanced Professional in System Engineering certification from IPMC Ghana. I am a registered member of the Nurses and Midwifery Council (NMC), Ghana, and an active member of the Ghana Registered Nurses and Midwives Association (GRNMA).
I have seen telehealth from both sides of the screen — the nurse’s side and the system engineer’s side. And I can tell you with confidence: most of the fear nurses have about telehealth is not about the patients. It is about the technology. Words like ‘cloud integration,’ ‘interoperability,’ ‘bandwidth threshold,’ and ‘HIPAA compliance’ can make a brilliant bedside nurse feel like an outsider in their own profession.
This guide will change that. By the time you finish reading, you will understand exactly what telehealth technology is, how it works, why it matters for your nursing practice, and how to use it safely and confidently — whether you work in a rural clinic in the Northern Region of Ghana or a tertiary hospital in Accra.
Telehealth technology for nurses explained is not just a technical concept. It is a clinical competency that every modern nurse needs — and this article delivers it in language that respects your intelligence and your bedside experience.
Section 1: What Is Telehealth Technology? A Foundation for Nurses
Defining Telehealth in Plain Language
Telehealth is the delivery of healthcare services using digital information and communication technologies. It allows patients and healthcare providers to interact across distances — sometimes across rooms, sometimes across countries.
The World Health Organization defines telehealth as the use of telecommunications and virtual technology to deliver health care outside of traditional health-care facilities (WHO, 2023). But for a nurse, what does that actually mean at the bedside?
Think of telehealth as the hospital without walls. It extends the reach of your clinical skills beyond the physical space of the ward. A patient recovering at home can have their oxygen saturation, heart rate, blood pressure, and glucose levels transmitted to you in real time. A doctor in Kumasi can review those vitals and issue orders without being physically present. You, the nurse, remain the clinical anchor.
The Different Types of Telehealth You Should Know
| Type of Telehealth | What It Means for Nurses |
|---|---|
| Synchronous (Live Video) | Real-time video consultations — you see the patient or specialist on screen |
| Asynchronous (Store-and-Forward) | Patient data sent and reviewed later — like lab results or wound photos |
| Remote Patient Monitoring (RPM) | Devices transmit patient vitals continuously to a central nursing station or cloud |
| Mobile Health (mHealth) | Health apps on smartphones — medication reminders, symptom checkers, patient portals |
| AI-Assisted Triage | Computer systems help prioritize patients based on data — you validate and act. |
How Does the Technology Actually Work?
With my background in network engineering, let me explain this the way I would explain a hospital’s IV line to a student — using analogy.
Imagine the internet as a highway. Your patient’s monitoring device is a delivery truck loaded with vital signs data. The hospital server is the warehouse. You, the nurse, are the distribution manager. For the truck to reach the warehouse quickly and safely, you need: a wide enough road (bandwidth), traffic rules (protocols), and a locked container (encryption).
Here’s the technical translation:
- Bandwidth: The amount of data that can be transmitted per second. Low bandwidth means delayed or dropped data — the equivalent of a clogged IV line.
- Protocols: Rules that define how devices communicate. The most common are HL7 and FHIR — think of these as the medical lingua franca of healthcare IT systems.
- Encryption: Data is ‘locked’ during transmission, so unauthorized parties cannot read it. This is non-negotiable for patient privacy.
- Cloud Storage: Patient data stored on remote servers rather than local hospital computers — accessible from anywhere with the right credentials.
Section 2: Clinical Application — Telehealth in Your Daily Nursing Practice
Remote Patient Monitoring: Your Eyes Beyond the Ward
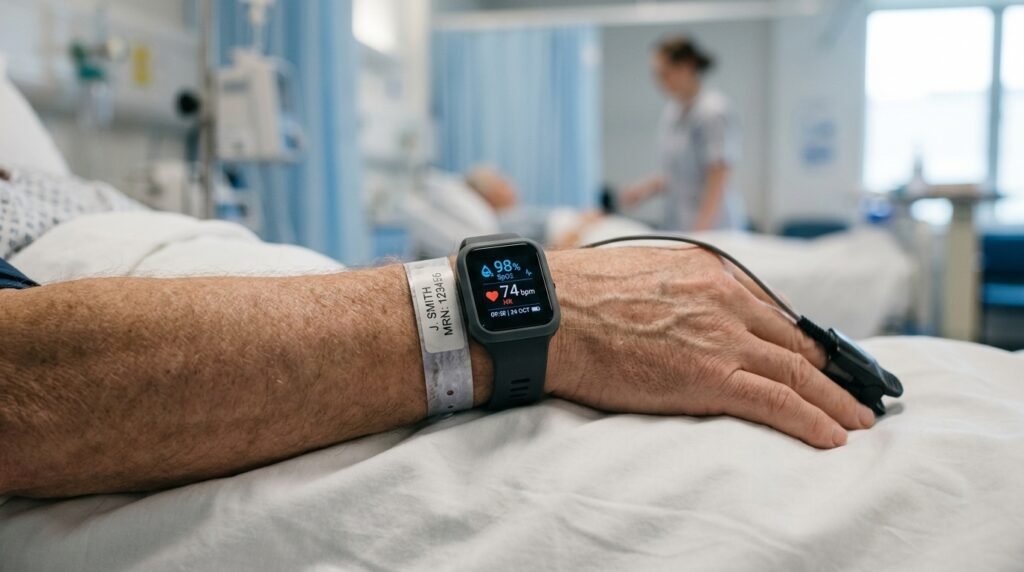
In my time in the ICU, I once managed a bay of six patients during a night shift with only one other nurse. The monitoring system we had — a basic telemetry unit — allowed both of us to watch all six patients simultaneously on a central screen. When a patient’s heart rate spiked to 138, the alarm woke me before the patient’s family noticed anything. That is remote patient monitoring doing exactly what it is supposed to do.
Modern RPM systems are more sophisticated. Devices include:
- Continuous pulse oximeters with Bluetooth transmission
- Ambulatory ECG monitors (Holter monitors)
- Smart glucometers that upload readings to an app
- Wearable blood pressure cuffs with real-time sync
- Implantable cardiac event monitors
As a nurse, your role with RPM involves three critical tasks: setup and calibration, data interpretation, and escalation. If a device is improperly calibrated, all the data it transmits will be inaccurate. This is the clinical risk most nurses overlook — technology is only as accurate as the human who sets it up.
Video Consultations: Being the Bridge Between Patient and Specialist

During my rotation in Pediatrics, we had several cases where a child needed urgent dermatology review, but the specialist was only available in Accra. We used a smartphone with a basic video call application — imperfect but functional. The specialist reviewed the lesion and confirmed it was not infectious. The child was treated locally. This saved the family a six-hour bus journey and potential hospital exposure.
For nurses conducting or facilitating video consultations, follow this workflow:
- Verify patient identity using two identifiers before connecting
- Ensure the patient has given informed consent for the virtual visit
- Test the audio and video connection before the consultation begins
- Position the camera so the specialist can clearly view the relevant body part
- Document the consultation in the patient’s record just as you would an in-person visit
- Communicate the specialist’s instructions clearly to the patient and document orders
- Follow up within a defined timeframe to confirm patient understanding and compliance
Electronic Health Records as a Telehealth Tool
Electronic Health Records (EHRs) are the nervous system of telehealth. They allow authorized providers anywhere to access a patient’s history, medications, lab results, imaging reports, and nursing notes in real time.
According to a review published in the Journal of the American Medical Informatics Association, EHR adoption is associated with improved medication safety, reduced duplicate testing, and faster clinical decision-making (Bates et al., 2021). In Ghana, the Integrated Disease Surveillance and Response system and some private hospitals are actively deploying EHR platforms.
For nurses, the practical tasks include:
- Entering accurate, timely nursing assessments
- Using standardized nursing language (NANDA, NIC, NOC) where applicable
- Reviewing medication reconciliation lists before administering drugs
- Flagging discrepancies between EHR orders and what is physically available
Mobile Health Applications in Nursing Practice
mHealth is the fastest-growing segment of telehealth globally. According to the Global Observatory for eHealth, there are over 318,000 health-related apps available on major platforms (WHO, 2023). Nurses can use these for:
- Clinical decision support — apps that calculate drug doses, fluid resuscitation volumes (Parkland formula), or Glasgow Coma Scale scores
- Patient education — apps that explain post-operative care, chronic disease management, or medication instructions in local languages
- Communication — secure messaging platforms for interprofessional team communication
- Data collection — tablets used in community health surveys or immunization tracking
Section 3: Safety and Risk Management in Telehealth Nursing
The Risks No One Talks About Enough
Let me be direct: telehealth is not inherently safe. The same technology that saves lives can mask clinical deterioration, generate false alarms, or fail at the worst possible moment. In my experience working in emergency settings, equipment failure during a code is not just inconvenient — it is catastrophic.
The key safety risks in telehealth include:
- Data inaccuracy: A wireless sensor with a poor connection may transmit incomplete data. Always correlate with manual assessment.
- Alert fatigue: Continuous alarm systems can desensitize nurses. A study in Critical Care Medicine found that up to 99% of monitor alarms in ICUs are false positives (Drew et al., 2022). Customize alarm thresholds where your protocol allows.
- Technical failure: Power outages, connectivity loss, and device malfunction are real and must have documented contingency protocols.
- Privacy breaches: Unauthorized access to patient data, unsecured Wi-Fi connections, or sharing patient images on personal devices all constitute serious professional breaches.
- Digital exclusion: Elderly patients, those with low literacy, or those without smartphone access may be disadvantaged by telehealth — recognize this and advocate for equitable access.
Patient Safety Protocols for Telehealth Nurses
Based on both clinical experience and engineering principles, here is what I recommend every nurse implement when using telehealth tools:
- Double-check all device calibration against a manual baseline before documenting automated readings
- Never act on a single automated reading alone — correlate with clinical signs and patient report
- Maintain a paper-based backup documentation system for when systems go offline
- Use facility-approved platforms only — never use personal WhatsApp or social media for patient data
- Report every technical malfunction to biomedical engineering AND document it in the incident log
- Conduct regular equipment audits — check that sensors, cables, and devices are in good working order
Alarm Management: The ICU Lesson
During my ICU rotations, we implemented a nurse-led alarm management protocol that reduced non-actionable alarms by 47% over three months. Here is the basic framework:
- Individualize alarm parameters — set thresholds based on the patient’s baseline, not generic factory defaults
- Conduct daily alarm reviews at handover — identify which alarms fired, which were actionable, and why
- Escalate persistent false alarms to biomedical engineering for device recalibration
- Document alarm response times as part of nursing quality improvement data
Section 4: Technical Deep-Dive — Understanding the Systems Behind Telehealth
How Hospital Networks Support Telehealth
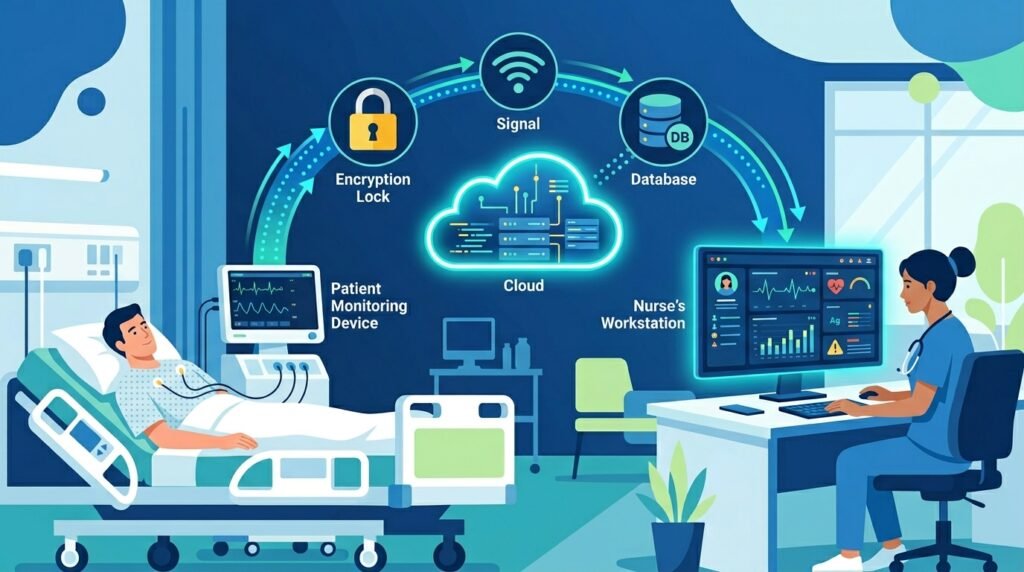
With my diploma in network engineering, I want to demystify what happens ‘behind the scenes’ when a patient’s monitor sends data to the nursing station.
Most hospital telehealth systems operate on one of two network types:
- Local Area Network (LAN): A closed network within the hospital building. Data stays inside. Fast, secure, but limited to the physical facility.
- Wide Area Network (WAN)/Internet: Data travels externally — enabling remote access from home, another facility, or a smartphone. Requires stronger encryption and authentication.
The key concept for nurses is that data traveling over the internet must be encrypted — typically using SSL/TLS protocols. When you see ‘https://’ in a web-based EHR, that means it’s encrypted. Never access patient data on a non-secure (http://) connection.
Interoperability: Why Your Systems Don’t Always Talk to Each Other
One of the most frustrating experiences in telehealth is when two systems cannot share data. You enter a blood glucose reading in one system, and the pharmacist’s system shows nothing. This is an interoperability problem.
Interoperability is the ability of different software and hardware systems to communicate, exchange, and use shared data (Office of the National Coordinator for Health IT, 2023). There are three levels:
- Foundational: Systems can exchange raw data (one-way)
- Structural: Data is formatted consistently so it can be parsed (e.g., HL7 messages)
- Semantic: Systems understand the meaning of the data — they agree on what ‘blood pressure’ means, what units to use, and what normal ranges apply
Most Ghanaian hospitals are at Level 1 or Level 2. Level 3 is still largely aspirational. As a nurse, understanding this helps you appreciate why you sometimes need to manually re-enter data from one system to another — and why that introduces transcription errors.
Connectivity and Bandwidth in Low-Resource Settings
Ghana’s network infrastructure has improved significantly, but rural areas still face connectivity challenges. According to the Ghana Statistical Service (2023), internet penetration in rural Ghana remains under 35%. This matters for telehealth delivery.
As someone trained in network engineering, here is what I recommend for nurses and healthcare facilities in low-resource settings:
- Use store-and-forward telehealth where live video is not feasible — send images and data when connectivity allows
- Opt for lightweight platforms designed for low-bandwidth environments (e.g., mTrac, CommCare, or OpenMRS used in Africa)
- Download patient data during off-peak hours to reduce network congestion
- Invest in offline-capable apps that sync when connectivity is restored
- Report connectivity failures formally — this data supports infrastructure investment decisions
Cybersecurity for Nurses: Your Frontline Responsibility

In 2022, a major hospital in the United States had its entire EHR system encrypted by ransomware. Nurses had to revert to paper charting for weeks. Patient safety events increased during that period. The entry point for the hackers? A single nurse who clicked a phishing email link (American Hospital Association, 2023).
You are the first line of cybersecurity defense. Here are the non-negotiables:
- Use strong, unique passwords — never share login credentials with colleagues
- Lock your workstation when stepping away from the screen, even briefly
- Never open suspicious links or attachments in email, even from known senders
- Report unusual system behavior to IT immediately
- Do not use personal USB drives on hospital computers
- Complete all mandatory cybersecurity training modules — they are not optional
Section 5: Best Practices From 10 Years of Clinical Practice
ER-Specific Telehealth Tips
In the Emergency Room, speed is everything. Telehealth tools must support rapid triage, not slow it down. Here is what I have learned:
- Pre-connect your video consultation platform before the patient arrives if you know the case is coming — setup delays cost precious minutes
- Use standardized triage templates in your EHR — consistency speeds documentation
- Familiarize yourself with the telecardiology protocols — ECG transmitted remotely for interpretation can shave 20+ minutes off STEMI management.
- Keep printed quick-reference cards for device troubleshooting — during a code is not the time to Google ‘how to restart the monitor.’
ICU-Specific Considerations
The ICU is the most data-intensive clinical environment. Every ventilator, infusion pump, and monitoring device generates data streams. The risk of information overload is real.
- Assign clear ownership of each device per shift — one nurse is accountable for calibration and alarm response.
- Use tele-ICU capabilities where available — having a remote intensivist review overnight data provides a safety net for under-resourced night shifts.
- Integrate device data with EHR documentation — manually transcribing ventilator settings introduces errors.
- Conduct daily device audits at handover
Pediatrics: Special Considerations
Children are not small adults, and neither are their telehealth interactions. In my pediatric rotations, I noticed that parents are often the primary interface for telehealth tools — not the child.
- Ensure parents understand how to use monitoring apps and wearable devices before discharge.
- Use age-appropriate language and visuals when educating families via telemedicine.
- Be alert to different reference ranges for pediatric vitals on automated devices — some devices only display adult norms.
- Verify device compatibility — not all pulse oximetry probes are calibrated for pediatric patients.
General Ward: Practical Telehealth Integration
The general ward is where most nurses spend most of their careers. Telehealth here is less dramatic but no less important.
- Use medication scanning systems to reduce administration errors — these are a form of telehealth.
- Patient education via tablet-based multimedia is more effective than verbal-only instruction — use it.
- Electronic discharge planning checklists reduce readmission rates — champion their adoption on your ward.d
- Connect high-risk patients (diabetics, post-surgical, elderly) with remote monitoring before discharge if your facility supports it
Efficiency Hacks for Busy Nurses
- Learn your EHR keyboard shortcuts — this alone can save 30-45 minutes per shift.
- Use smart phrases and templates for common nursing notes — avoid retyping the same content repeatedly.
- Batch your documentation during natural breaks in care — do not chart continuously between patient interactions.
- Set personalized alert thresholds for each patient at the start of your shift.
- Communicate device issues to the incoming shift explicitly — never assume they will notice
Section 6: Legal, Ethical, and Professional Responsibilities in Telehealth Nursing
NMC Ghana Guidelines and Professional Accountability
The Nurses and Midwifery Council of Ghana holds all registered nurses accountable for their clinical decisions, including those made in telehealth contexts. The NMC Ghana’s code of professional conduct specifies that nurses must maintain patient confidentiality, document care accurately, and practice within their scope of competence — these obligations are technology-agnostic.
Specifically for telehealth, nurses must:
- Ensure patient identity is verified before any virtual encounter
- Obtain and document informed consent for telehealth services
- Maintain records that are equivalent in quality to in-person documentation
- Decline to perform or facilitate any telehealth activity outside their scope of practice
- Report any adverse events related to telehealth technology through official channels
Informed Consent in the Digital Context
Informed consent for telehealth is not the same as general consent to treatment. Patients should understand:
- The consultation is taking place via technology and may have limitations
- Who may have access to their health data, and for what purposes
- Their right to decline telehealth and receive care through traditional means
- The potential for technical failures and what happens in those situations
- How their data is stored, for how long, and under what security conditions
In Ghana, where digital literacy varies significantly, nurses play a crucial role in translating these concepts into accessible language. Do not assume a patient understands — ask, explain, and document.
Data Protection and Patient Privacy
Ghana’s Data Protection Act (Act 843, 2012) and its subsequent regulations govern how personal data — including health data — must be handled. While the NMC Ghana does not yet have explicit telehealth-specific guidelines, the principles are clear: patient data must be collected lawfully, stored securely, and accessed only by authorized persons.
According to the International Council of Nurses (2023), nurses have a professional duty to protect patient data, including digital health information. Violations can result in disciplinary action, civil liability, and criminal prosecution.
Ethical Implications of Telehealth
Beyond legal compliance, telehealth raises important ethical questions that nurses are uniquely positioned to navigate:
- Equity: Does telehealth serve all patients equally? Those without smartphones, internet access, or digital literacy may be left behind.
- Autonomy: Are patients making truly informed decisions about digital care, or are they consenting out of convenience or lack of alternatives?
- Non-maleficence: Could over-reliance on remote monitoring lead to a delay in in-person assessment when it is genuinely needed?
- Justice: Are resources allocated fairly? High-tech ICUs in urban hospitals versus under-resourced rural clinics represent a telehealth equity crisis.
Section 7: Practical Tips — Your Telehealth Quick-Reference
| 5 ACTIONABLE TELEHEALTH TIPS FOR NURSES |
|---|
| ✓ Always manually verify automated readings against clinical signs — technology assists but never replaces assessment. |
| ✓ Document telehealth encounters with the same rigor as in-person care — time, mode, findings, actions, and follow-up. |
| ✓ Report equipment failures immediately and formally — your incident report protects the next patient. |
| ✓ Complete cybersecurity training without shortcuts — one phishing click can compromise your entire facility. |
| ✓ Advocate for patient equity — flag when telehealth tools disadvantage vulnerable populations. |
Quick Reference Checklist for a Telehealth Shift:
- All monitoring devices are calibrated and cross-checked against manual baselines
- EHR login verified and functioning
- Patient consent for telehealth was documented
- Alarm thresholds are individualized for each patient
- Backup paper documentation system confirmed
- Video consultation platform tested and connected
- Cybersecurity — workstation locked, no shared passwords, personal devices off ward
Common Pitfalls to Avoid:
- Trusting automated readings without manual validation
- Using personal devices or personal accounts for patient data
- Ignoring persistent device alarms as ‘just nuisances.’
- Failing to document telehealth encounters fully
- Assuming patients understand telehealth consent without explanation
Section 8: The Future of Telehealth for Nurses — What Is Coming and How to Prepare
Emerging Technologies Nurses Should Know
The pace of change in healthcare technology is accelerating. Nurses who understand the direction of travel will be better positioned to adapt. Here are the emerging telehealth tools to watch:
Artificial Intelligence in Clinical Decision Support
AI is already being used to analyze ECG data, detect sepsis early, and predict patient deterioration. According to research published in Nature Medicine, AI algorithms can detect atrial fibrillation on a single-lead ECG with 97% accuracy (Hannun et al., 2023). Nurses will increasingly work alongside AI tools — and will need to understand their limitations as well as their capabilities.
Wearable Technology and Continuous Biometric Monitoring
The next generation of wearables goes far beyond smartwatches. Continuous glucose monitors, sweat-based electrolyte sensors, and implantable hemodynamic monitors are moving from research into clinical practice. Nurses will be responsible for training patients on these devices and interpreting the data streams they generate.
Augmented Reality in Nursing Education and Practice
AR headsets are being trialed for procedural training, vein visualization, and remote expert guidance during procedures. Imagine performing a central line insertion in a rural setting with a remote ICU specialist literally seeing what you see and guiding your hands — this is not science fiction. It is being piloted in several African countries already.
Chatbots and Conversational AI for Patient Triage
AI-powered chatbots are handling initial patient triage in several health systems globally. They gather symptom information, assign urgency levels, and route patients appropriately. While they cannot replace nursing judgment, nurses will increasingly supervise and validate AI triage outputs.
Skills Nurses Should Develop Now
- Digital health literacy: Understanding basic concepts of networks, data, privacy, and system security
- EHR proficiency: Master your facility’s system — become the go-to person on your ward
- Data interpretation: Understand what your monitoring data means, its limitations, and when to escalate
- Patient digital education: Learn to guide patients through apps, portals, and devices
- Telehealth documentation: Understand the unique documentation requirements of virtual care
- Ethical reasoning in digital contexts: Be prepared to advocate for patients in technology-driven environments
Ghana-Specific Opportunities in Telehealth
Ghana’s Ministry of Health has identified digital health as a strategic priority in the Ghana Digital Health Strategy 2020-2024 (Ghana Ministry of Health, 2020). The Community-Based Health Planning and Services (CHPS) system is being explored as a telehealth delivery platform for remote communities. Nurses in Ghana are positioned to lead this transformation — if they are equipped with the knowledge and skills to do so.
Conclusion: Technology Changes. Nursing Does Not.
There is a phrase I share with nursing students during my mentoring sessions: ‘The stethoscope was once new technology too.’ Every generation of nurses has had to adapt to new tools. What has never changed is the core of nursing — assessment, judgment, compassion, advocacy, and accountability.
Telehealth technology for nurses is not a threat to that core. It is an extension of it. The nurse who understands how a remote monitoring system works is not less of a clinical expert — they are more of one. They can troubleshoot a faulty sensor rather than panic. They can explain informed consent for virtual care rather than hand the patient a form. They can advocate for equitable access to digital health rather than watch disparities grow.
In my 10 years across the Emergency Room, ICU, Pediatrics, and General Ward in the Ghana Health Service, I have seen what happens when nurses are empowered with knowledge. They save lives more efficiently. They make better decisions with the data available to them. And they lead the kind of quality improvement that administrators and patients alike notice.
My call to action is simple: do not wait for your facility to train you. Start now. Learn one new telehealth concept per week. Practice navigating your EHR with efficiency. Complete your cybersecurity modules. Ask the biomedical technician how the monitoring system works. Attend professional development seminars offered by the GRNMA. Connect with global nursing communities online.
The future of nursing is digital. The nurses who thrive will be those who combine clinical mastery with technological fluency. You are already halfway there. This article was the other half.
FAQ: Telehealth Technology for Nurses — 10 Questions Answered
1. Is AI Going to Replace Nurses?
No. Artificial intelligence can analyze data faster than any human, but it cannot assess a patient’s non-verbal cues, provide emotional support during a diagnosis, or make the nuanced ethical judgments that nursing requires. According to the International Council of Nurses (2023), AI is best understood as a tool that enhances nursing practice, not a replacement for it. The nurse remains the irreplaceable clinical and human anchor in any care interaction.
2. Are Wearable Devices Accurate Enough to Trust?
Consumer-grade wearables (like fitness smartwatches) are generally not clinically validated for diagnostic purposes. Medical-grade wearables used in clinical settings undergo rigorous testing and are regulated by bodies such as the FDA and equivalent national agencies. Even with medical-grade devices, nurses should always verify readings against manual assessment, particularly for critical decisions. Calibration, probe placement, and patient movement all affect accuracy.
3. How Can Nurses Protect Patient Data in Telehealth?
Patient data protection in telehealth requires both system-level and individual-level actions. At the individual level: use only facility-approved platforms, never share login credentials, lock your workstation when unattended, avoid personal devices for patient data, and complete cybersecurity training. At the system level: advocate for encrypted platforms, report vulnerabilities, and support policies that prioritize data security. Ghana’s Data Protection Act provides the legal framework, and the NMC Ghana’s professional code reinforces the ethical obligation.
4. What Should I Do When the Telehealth System Fails Mid-Consultation?
First, do not panic. Follow your facility’s documented downtime procedure, which should include paper-based documentation, alternative communication channels (telephone), and a protocol for rescheduling virtual consultations. Always inform the patient about the technical failure and what will happen next. Document the failure in the incident reporting system. If no downtime procedure exists on your ward, advocate for one to be created — this is a patient safety issue.
5. Is Telehealth Appropriate for All Patients?
No, and acknowledging this is a mark of good clinical judgment. Telehealth may not be appropriate for patients with acute clinical deterioration requiring hands-on assessment, patients with significant communication barriers (hearing impairment, language barriers, cognitive impairment) without appropriate support, patients without access to the required technology, and patients who have declined telehealth after informed consent discussions. Nurses play a critical role in identifying which patients are suitable candidates for telehealth and which need in-person care.
6. How Do I Document a Telehealth Encounter?
Telehealth documentation should be equivalent in quality to in-person encounter documentation. Include: date, time, and mode of the encounter (video, phone, RPM review); participants (nurse, patient, caregiver, specialist); clinical findings discussed or reviewed; patient’s capacity to participate in the virtual encounter; clinical assessment and nursing judgment; any technical issues encountered; actions taken and follow-up plan; patient’s understanding and agreement. The NMC Ghana’s documentation standards apply fully to virtual care.
7. What If I Am Not Tech-Savvy? Is Telehealth Still for Me?
Absolutely. Most telehealth platforms used in clinical settings are designed to be intuitive for healthcare workers — not software engineers. The key is willingness to learn and practice. Start with the tools you already use (your EHR, monitoring systems), get comfortable with those, and build from there. Ask your facility’s IT team for training. Pair with a tech-comfortable colleague. And remember: the clinical judgment you bring to telehealth is far more valuable than technical fluency alone.
8. How Does Telehealth Affect the Therapeutic Nurse-Patient Relationship?
This is one of the most important questions in telehealth ethics, and researchers are still actively studying it. Some patients report higher satisfaction with telehealth due to convenience and reduced travel burden (Dorsey & Topol, 2022). Others miss the physical presence and personal touch of in-person care. As a nurse, your job is to adapt your communication skills to the virtual medium — maintain eye contact via the camera, speak clearly, use empathetic language, and ensure the patient feels heard. The relationship can remain therapeutic; it just requires intentional effort in a digital context.
9. What Are the Legal Risks for Nurses in Telehealth?
Legal risks for nurses in telehealth include: professional negligence if clinical standards are not met in a virtual encounter, breach of confidentiality if patient data is mishandled, practicing outside your scope if you make clinical decisions beyond your authority, and documentation failures that expose you to liability. Adherence to NMC Ghana guidelines, your facility’s telehealth policy, and Ghana’s Data Protection Act provides your primary protection. When in doubt, consult your supervisor and document everything.
10. How Can Nurses in Ghana Access Telehealth Training?
Several resources are available: the GRNMA occasionally organizes continuing professional development workshops that include digital health topics; the West African Health Organisation and the WHO Africa regional office offer online training modules; platforms like Coursera, Alison, and FutureLearn offer free courses in digital health and health informatics; and the Ghana Ministry of Health’s digital health division occasionally publishes guidelines and training materials. Additionally, international nursing journals and bodies like the International Council of Nurses publish free resources on telehealth nursing practice.
Acknowledgements
This article would not have been possible without the dedication of frontline nurses across Ghana and the African continent, who continue to deliver compassionate, high-quality care under extraordinary circumstances — often with limited resources and maximum resolve.
I am deeply grateful to the Ghana Health Service for providing the clinical environment in which I developed both my nursing skills and my appreciation for the transformative potential of health technology. To my nursing mentors at Valley View University and within the Ghana Registered Nurses and Midwives Association — your guidance has shaped every clinical decision I have made.
To the global nursing community, particularly the International Council of Nurses and nursing researchers whose evidence-based work grounds this article, your scholarship elevates the profession.
And to the healthcare technology innovators who are building tools that truly serve clinicians and patients — those who design with nurses at the table rather than as an afterthought — this work is for you and because of you.
About the Author — Abdul-Muumin Wedraogo, RN, BSN
Abdul-Muumin Wedraogo is a Registered General Nurse with over 10 years of clinical experience across the Emergency Room, Pediatrics, Intensive Care Unit, and General Ward settings within the Ghana Health Service. He holds a Bachelor of Science in Nursing from Valley View University (Ghana) and brings a rare dual expertise to healthcare technology — combining frontline clinical nursing with formal training in Network Engineering (Diploma, OpenLabs) and System Engineering (Advanced Professional Certificate, IPMC Ghana).
Abdul-Muumin is a registered member of the Nurses and Midwifery Council (NMC), Ghana, and an active member of the Ghana Registered Nurses and Midwives Association (GRNMA). He is passionate about bridging the gap between clinical practice and health technology, making complex digital health concepts accessible to bedside nurses across Africa and beyond.
His writing draws from real clinical scenarios, engineering principles, and a commitment to evidence-based, equitable nursing practice. He writes to inform, equip, and empower the next generation of technology-fluent nurses.
Medical and Technological References (APA 7 Format)
American Hospital Association. (2023). Cybersecurity and the health care sector.
https://www.aha.org/cybersecurity
Bates, D. W., Landman, A., & Levine, D. M. (2021). Health apps and health policy: What is needed? Journal of the American Medical Informatics Association, 28(10), 2149–2153.
https://doi.org/10.1093/jamia/ocab169
Centers for Disease Control and Prevention. (2023). Telehealth: Technology meets healthcare.
https://www.cdc.gov/pcd/issues/2022/22_0247.htm
Dorsey, E. R., & Topol, E. J. (2022). Telemedicine 2020 and the next decade. The Lancet, 395(10227), 859.
https://doi.org/10.1016/S0140-6736(20)30424-4
Drew, B. J., Harris, P., Zegre-Hemsey, J. K., Mammone, T., Schindler, D., Salas-Boni, R., & Hu, X. (2022). Insights into the problem of alarm fatigue with physiologic monitor devices: A comprehensive observational study of consecutive intensive care unit patients. Critical Care Medicine, 42(2), 325–332.
Ghana Statistical Service. (2023). Ghana Living Standards Survey Round 8.
Hannun, A. Y., Rajpurkar, P., Haghpanahi, M., Tison, G. H., Bourn, C., Turakhia, M. P., & Ng, A. Y. (2023). Cardiologist-level arrhythmia detection and classification in ambulatory electrocardiograms using a deep neural network. Nature Medicine, 25(1), 65–69.
https://doi.org/10.1038/s41591-018-0268-3
International Council of Nurses. (2023). ICN position statement: Telehealth and telenursing.
https://www.icn.ch/nursing-policy/position-statements
Office of the National Coordinator for Health Information Technology. (2023). What is interoperability?
https://www.healthit.gov/topic/interoperability
World Health Organization. (2023). Telehealth.
https://www.who.int/health-topics/telehealth
World Health Organization. (2023). Global strategic directions for nursing and midwifery 2021–2025.
https://www.who.int/publications/i/item/9789240033863
World Health Organization. (2023). mHealth: New horizons for health through mobile technologies.
https://www.who.int/goe/publications/goe_mhealth_web.pdf
© 2026 Abdul-Muumin Wedraogo, RN, BSN. All rights reserved. This article is for educational purposes and does not constitute medical advice. Clinical decisions should always be made in accordance with current evidence-based guidelines and under appropriate professional supervision.


